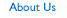Enhancing the Health Care Client Installation Experience
Introduction
"Profit equals revenue from continuously happy clients, minus costs."
This notion, quoted from Tom Peter's book, Thriving on Chaos, seems simple to understand and implement. But the processes by which Health Plans gain new clients, renew others, make them 'happy' at the outset and derive ongoing profit from the resulting stable client base are often very challenging and complex.
Peters' central theme is 'continuously happy clients.' Happy clients stay loyal to the Health Plan and its products, provide a stable recurring revenue stream and reduce the need to sell replacement business due to client turnover or "churn." The lower level of client churn reduces the Plan's cost of sales in the aggregate and on a per-member and per-dollar-of-premium or premium-equivalent basis - all leading to increased profits or surplus.
To have 'continuously happy clients' a Health Plan should ensure that each client begins its initial relationship with the Plan in a positive way, one that satisfies them, makes them 'happy.' Then, through ongoing initiatives such as new product features, aggressive pricing, web-based information services, upgraded call/contact centers, wellness programs and others, the Plan can work at keeping the clients 'continuously happy.'
Based on our considerable experience in this area, Questas' premise for this monograph is that many Health Plans:
- Do not subscribe to the old adage - "the first impression is the lasting impression" - in an institutional fashion
- Have not formalized processes in a manner that ensures that each client's first operational encounter with the Plan is truly the beginning of a 'happy' relationship
- Do not manage and measure the end-to-end process of installing new and renewing existing clients, have little idea about how their clients feel about the process and do not ascertain on a regular basis the downstream effects their unhappy clients are having on the Plan's operating success.
Thus, we believe, many Health Plans begin or renew client relationships in an unsatisfactory manner - setting them up to terminate at their first or next anniversary date.
This monograph discusses the ways in which Health Plans currently install new and renew existing clients, the problems often associated with their approaches, the basic components of a successful program and some implementation considerations for, and benefits to be derived from, remedying the existing situation.
Executive Summary
The activities by which a Health Plan installs new, and renews existing, clients begin in the marketplace, span several Plan operating units, and are completed and enshrined in the Plan's core processes and systems that provide or support the services the client has contracted to receive from the Plan.
Health Plans have different names for the process - some of which are:
- Client, or group, or account, set-up
- Client, or group, or account, installation
- 'On-boarding' clients
- Group set-up and member enrollment
- Business acquisition and renewal
- Case installation, or
- Other
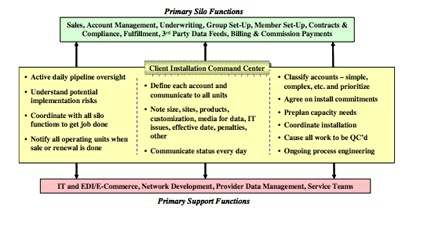
For convenience, we will use 'Client Installation' as the process name throughout this monograph. A block diagram that depicts the typical key elements of the Client Installation process appears below.
Many Health Plans do not overtly manage and measure the work in and results derived from the collection of silo processes that comprise Client Installation. Instead, they rely on their 'well-intentioned staff' to assure them that their collective efforts will yield positive timely results. Such Plans run the risk of performing the tasks incorrectly, incompletely and/or late - to the detriment of their service reputation with new and existing clients.
When Client Installation processes are not done properly, completely and timely, there are visible failures that affect the client and the Plan - notable among them:
- Groups are billed improperly
- The Plan suffers cash collection & reconciliation problems
- Improper commissions are paid to brokers
- Performance penalties are paid to large groups
- Core Account, Member and Benefits data files/databases - are wrong
- Coverage and benefits data are not accessible to providers at the point-of-care
- Members might be unable to receive care
- Claims are adjudicated incorrectly
- Customer service cannot address benefits and other questions
- Unhappy groups lapse after 1 year or less - the high churn increases cost of sales and reduces account profitability
- Members lapse ("back-door losses") at an accelerated rate - reducing profit per member
- Lapsed groups and members - and unhappy brokers - negatively affect new sales
Conversely, when Client Installation processes are done properly, completely and timely, there are specific benefits that the Plan and its constituents enjoy - notably among them:
- Groups are billed and pay properly
- Properly paid brokers are happy
- The Plan pays no performance penalties related to Client Installation
- Core databases are accurate
- Providers can check eligibility, benefits & coverage at point-of-care
- Members have access to care as designed
- Claims adjudicate as designed
- Customer service interventions are fewer in number, higher in quality
- Happy groups and members remain with the Plan over time - less churn, lower cost of sales, higher profits
- Happy groups, members & brokers are missionaries for new clients - the source for new revenues and profits
Plans that accomplish client installations well usually:
- Focus on client installation activity as a discrete horizontal process
- Assign accountability, responsibility and authority to accomplish the program well to a single entity - a Process Owner, a Program Management Office or a War Room
- Measure the results and look for ways to continuously improve the program.
On seven (7) past occasions, Questas' consultants have helped medium- and large-sized health plans significantly improve this process:
- In one instance for a large Blue Cross Blue Shield Plan
- In another, installing and operating four standalone national shared services centers for a large nationwide multi-line insurer
- On two occasions, installing and operating separate solutions for geographically dispersed regions of a large HMO.
All of these Plans experienced significant improvements in process management, service and financial results and client satisfaction.
If your Plan is suffering from any of the problems noted above, or if you suspect that your current Client Installation program is or is about to become problematic and/or it will not scale with an increase in volume, then please read on.
If you would like to discuss this monograph further or determine how Questas could assist your Plan in these matters, please contact Questas by e-mail at client-installation@questas.net or by telephone at 212.229.0498.
This monograph can also be viewed at and downloaded from the Questas website at www.questas.com.
The Current State - Installing New, and Renewing Existing, Clients
The activities by which a Health Plan installs new, and renews existing, clients begin in the marketplace, span several Plan operating units, and are completed and enshrined in the Plan's core processes and systems that provide or support the services the client has contracted to receive from the Plan.
Health Plans have different names for the process - some of which are:
- Client, or group, or account, set-up
- Client, or group, or account, installation
- 'On-boarding' clients
- Group set-up and member enrollment
- Business acquisition and renewal
- Case installation, or
- Other
For convenience, we will use 'Client Installation' as the process name throughout this monograph. A block diagram that depicts the typical key elements of the Client Installation process appears below.
Process aficionados would call this a horizontal (end-to-end) process that spans several vertical silo organizations of the Plan. This is different than a standalone process that would reside within a single organizational entity (or silo) of the Plan.
Let's first look at a brief overview of the sequence of events in Client Installation, which will later form the basis for our assessment of how Plans conduct the end-to-end process today:
- New Sales - The Plan's Sales team prospects in the market - alone or in conjunction with third parties like brokers, agents, benefits consultants and Web-based e-insurance agents - to develop a pipeline of potential new business accounts ("groups") and their employees, dependents and retirees. This is an ongoing process whereby the lead pipeline is populated and targeted according to the anniversary date that each prospective new client has with the Plan(s) with whom it has existing relationships. In a parallel process, Plans also sell to individuals - often called "non-group" business. The Plan might do this directly with individuals via telemarketing, Web-based services, direct marketing and through intermediaries like brokers and e-agents. The lead times for premium and fee quotes and client decisions often vary by client segment - self-insured (or ASO) and premium based - and by size: large, medium and small businesses and "non-group" or individual business.
- Renewals - The Plan tracks the anniversary dates of all of its existing clients. At a predetermined date, the Plan prepares and presents to each client a renewal package to facilitate its decisions about staying with the Plan for another year or more. In many cases, the Underwriting unit prepares these renewal packages and provides them to Sales or Account Management representatives to present to their clients (or to their brokers or benefits consultants). The time interval prior to each anniversary date that dictates when a renewal package is prepared and presented varies by market and by client segment: self-insured accounts might be 6-9 months or longer prior to anniversary; large and medium-sized premium accounts could be 90-120 days; small businesses and individuals could be as many as 90-120 or as few as 30 days or less.
- Client Decisions - Clients decide whether or not to initially buy or renew the Plan's offerings. This process is almost always accompanied by some degree of negotiation - of benefits, features, provider network coverage, prices, etc. In this decision cycle, the client also makes known its 'special' needs- for example, special circumstances for open enrollment periods (languages spoken, shifts to accommodate, etc.), customized ID cards and benefits booklets, special requirements surrounding electronic enrollment and ongoing eligibility maintenance, billing parameters and locations, whether or not they want to self-bill, desires for dedicated claims units (usually for large self-insured accounts), special provider network considerations, PBMs, etc. The Plan must determine if it can meet these needs operationally and profitably within the price it has quoted or if it will revise its quote.
If the client decides not to purchase or renew the Plan's offerings, the process stops. Some Plans then conduct a "post-mortem" assessment, that inspects lost business trends and root causes in order to improve on sales/renewal process.
If the client decides to purchase or renew the Plan's offerings, the final composite of product features and benefits, service requirements, and other matters (which, collectively, we call "the essence of the sale") are captured in a contractual document and signed by both parties. This approval process and, for insured entities, payment for the estimated first month's premium, usually kicks off the beginning of the client installation process and sets the times and dates for member marketing and the open enrollment period(s). - Member Marketing - once the group client has agreed to buy or renew the Plan's
offerings, and when or as the contract is being signed, the Plan conducts its open enrollment period with the account. Depending on the account, the open enrollment might be transparent, in which case the Plan openly markets to and competes for members; or it might be passive, in which case the account controls the flow of information that its employees, retirees and dependents see and the Plan representatives have little or no direct contact with the prospective or renewing members. Once member marketing is done, the open enrollment process is also completed - yielding some number of new or renewal applications for membership in the Plan. These could be on paper or other non-electronic medium; but, ideally, they would be captured electronically by the account or one of its benefit-related vendors.
Enrollment data can be sent to the Plan by many parties - and the list is growing every day; they include:
- The employer itself or its payroll or human resources technology vendor - like ADP, PeopleSoft or Oracle
- Brokers and/or managing general (insurance) agents - like Acordia
- Benefits consultants - like Hewitt, Wyatt, Towers Perrin, etc.
- Taft-Hartley funds
- And the growing list of significant Total Benefits Outsourcing firms and consortia - like Fidelity's FHRS unit, CitiStreet, Hewitt/Exult, Mercer/ Putnam, EDS/Towers Perrin, and others
- Conduct the post-sale underwriting check (if used by the Plan) - Once all
members applications are counted - prior to being loaded into the Plan's systems - some Plans elect to assess whether or not the total membership for a given account in a particular product or overall is in compliance with the underwriting guidelines that were set forth at the time of the sale or renewal. For example, some Plans specify a percentage of employee penetration that must be achieved in a particular product, or overall as part of a total account sale, in order for the prices/rates to remain as proposed; else the Plan would have the right to re-price accordingly. If that is the case, then such action is termed a "post-sale underwriting check."
If the post-sale check occurs and the client account is out of compliance with the original underwriting guidelines, the Plan could choose to re-price or reject the account. The account could then also choose to accept or reject the new price, cancel its contract and go elsewhere. If either party were to cancel the 'sale' the Client Installation process would cease at this point - Group Set-up - is comprised of several key processes that are based on materials - in the form of a signed proposal or contract and group paperwork (or electronic information) - that the Sales and Account Management teams (or, alternatively, the Underwriters) deliver to the operating unit(s):
- Create or Update Client Data - where the client's demographic data, organizational structures and related items are captured, usually in an account database or in an account structure within the membership database.
- Create or Update Benefits Data - This is usually the step where the operating
unit captures the essence of the sale - which entails translating key aspects of the contract - or signed proposal - into a format that can be used to set up the account and install its employees, retirees and dependents. In some Plans, the same contract is translated multiple times - by different internal organizations, for different reasons and, unfortunately, sometimes with different results.
In this instance the contract data are converted into specific structures for features, benefits and rules that will drive certain Plan processes - e.g., customer service inquiry responses regarding coverage and benefits; the development of certificates, contracts and employee handbooks; claims adjudication and other functions. In some Plans, this is considered a system configuration event ("config") and is done by the IT staff. In others, it is a grouping of business functions that are done by several organizations - benefits set-up and fulfillment for example. - Create or Update Billing and Commission Data - where the billing information and agreements for each Client are loaded into the policy/ membership administration and/or billing systems so the billing and collection processes can begin. The commission data are loaded into whatever system is used to pay commissions to the Plan's commissionable entities - internal and external agents, brokers and other distribution channels.
- Develop new contracts and certificates- this is a regulatory compliance function that often resides within a Plan's Legal unit. It exists whenever a Plan allows its own or third party agents to sell clients products, features and benefits for which the Plan must then obtain waivers to state filings or re-file its offerings with a Department of Insurance, or its equivalent, before such policies can be executed and serviced. This retroactive process is often very time-consuming (90-120 days or more in many cases) and must be well managed to occur in a reasonable time period. This discrete process does not exist in all Health Plans.
- Member Set-Up - is comprised of a number of key processes:
- Enroll new members or update eligibility data for renewing members - where, for non-electronic materials, member applications are screened, edited, quality-controlled and then loaded or used as the source for updates to member records in the Membership database. For electronic applications and maintenance items, the data files are often pre-screened to ascertain completeness and quality and then either rejected for excessive errors or accepted and processed. For electronic applications and maintenance items, the formats could still be customized and the Plan might agree to translate them; but increasingly, they are shifting to standardized HIPAA-compliant electronic transactions.
- Fulfillment - where the output requirements of the group and member
enrollment process are met, or "fulfilled," internally or via outsourced relationships with qualified vendors or both. Fulfillment processes entail the production and distribution of items such as: ID cards, benefits booklets, contracts and certificates, affiliated materials, etc. In some cases, the benefits information is fed electronically to an employer or its agent so an all-benefits information packet can be produced for employees, retirees and dependents - covering health care, dental, 401ks, pensions, cafeteria benefits, etc.
If third parties are used to develop and distribute fulfillment materials, the Plan sends the data to external fulfillment partners. In some cases, e.g., for ID cards and collateral materials, there are complex scheduling, coordination and quality control requirements that must be met with such third party vendors to assure successful results. - Synchronize data with important third party business partners - health care
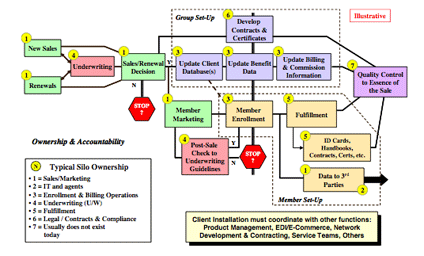
does not reside in a vacuum. It is one of several related benefits that employers might offer to employees, retirees and dependents; and which individuals in non-group settings purchase of their own accord. Thus, a Plan might offer separate products for dental care, vision and mental health/substance abuse. It might have a separate drug benefit serviced by its own or a third party pharmacy benefits manager (PBM). In some cases, the Plan might be a multi-line insurer and have to coordinate health care with other group products - life, ADD, etc. The Plan might offer a Consumer Directed Health Plan (CDHP) that incorporates a health savings account (HSA) that must be managed by a third party like a bank. In some instances, the Plan might offer a workers compensation product that creates an in-house Coordination of Benefits opportunity. And the Plan might need to provide patient rosters to capitated providers so they know which Plan members have elected to join their panels.
In such cases, the Plan must synchronize benefits, billing and/or enrollment data with its affiliated products and/or third parties. In most cases, the Plan should also synchronize all changes to its offerings as soon as they are made in the yearly planning cycle or on an ongoing basis.
The Client Installation process is not completed until the new and renewing members can receive all aspects of the care for which they or their employers have contracted - and that includes care delivered by all 'downstream' third parties. This is often a problematic issue for Plans and their partners.
- Quality Control - unlike the confirmations of securities' trades that are provided by
financial services firms, or confirmed itineraries from online travel agencies, the health care insurance sector does not confirm to its clientele that what they think they bought from the insurer is actually memorialized in the Plan's systems and processes.
Instead, Health Plans ...
- Install accounts - and their demographic, organizational, product and billing data; members and their demographic and sometimes billing and/or health risk assessment data; and product-related benefits data that determines how service is rendered and claims are adjudicated
- Create and deliver to clients items like ID Cards with embedded data, employee handbooks, contracts, certificates and other materials that both explain and determine how the member is to be serviced
- Do not usually quality control the information back to what the client thinks it bought - i.e., "the essence of the sale" - and do not require the client to confirm that its various account, member and product data now embedded in the Plan's systems are correct.
A formal Quality confirmation is a core process that we believe Plans need to consider embedding in their workflow. Early adopters will be positively differentiated from their competitors until the market moves more broadly in this direction.
Problems in Today's Client Installation Programs
The primary goal of the end-to-end Client Installation process is to assure that 100% of all cases ('accounts' or 'groups') and members are installed correctly and completely on or before their effective dates. In some sectors, e.g., for small businesses, this might not occur due to factors beyond the Plan's control - for example, brokers holding competing bids until the last possible moment before helping their small business client decide on the Plan. In those cases, the target installation date should be a mutually agreeable date beyond the anniversary or effective date for the account.
Many Plans do not measure this process - i.e., they do not determine the percentage of clients they install - completely and correctly - on or before their effective dates. Moreover, they do not manage the end-to-end process to cause such results to occur. Instead, they focus on managing the results in the discrete processes or sub-processes germane to a particular operating entity's domain or 'silo.' In many cases, they pay penalties to large insured and ASO accounts for failure to meet this service level.
Plan executives will argue, and it is true, that some Plans have been successful in installing clients by their effective dates without managing the end-to-end process from sales to the final third party data feeds. Some Plans rely on well-intentioned staff to assure their success. Others bulk up on overtime costs and otherwise push work through the pipeline. In many such cases, Plans 'meet the target installation dates' but later uncover process and data quality problems, caused in the Client Installation flow, that have created significant, lingering downstream problems in areas like billing, collection and reconciliation, claims processing, service and patients' receipt of timely care at the right sites. Importantly, an unmanaged process might not scale properly and cost-effectively as the Plan grows its account and membership base over time.
Problems in the end-to-end Client Installation process manifest themselves in ownership and accountability gaps, errors, unnecessary delays, excessive costs and other matters which we discuss in this section.
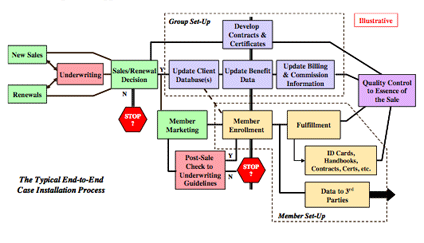
1. Ownership and Accountability for Results
As shown in the process map on the following page, the Client Installation process is comprised of a collection of discrete processes or activities, each of which is usually owned by a revenue generating or operational unit within the Plan. The work moves horizontally from left to right - i.e., from the marketplace and customers into the Plan, then into its core processes and systems, and on to third parties if they are part of the Plan's solution.
As work moves into and through a particular business unit, that unit might have a service metric for its portion of the work. For example, the member enrollment unit might promise 3-day turnaround on clean paper applications from date of receipt to the date on which all enrollment data are in the Plan's Membership Database. However, in our experience, it is rare that a Plan assigns an end-to-end owner for the full horizontal process or the results the market values - complete and correct installation on or before the effective date. In other words, in most Plans we have observed, no single person or business unit acts as the advocate for accounts and members to assure them this key process will be done correctly, completely and timely on their behalf. And this is often true even in Plans that have begun migrating to a process-focused business model.
As a result, we often observe the following problems:
- Silo goals take precedence over the horizontal process goals - and are reinforced by the performance management, compensation and rewards systems in place in the various silotic business units
- Clients (accounts or groups) and data are 'thrown over the walls' from silo to silo - without regard for the effects of one unit's work on the next. This 'workbench' method of processing seeks to make each sub-process work for the unit doing it without regard for the timeliness, quality and cost of the end-to-end process
- End-to-end results are not managed and might not be measured - preventing the Plan from understanding how well or poorly it is impressing its new clients and serving its renewing clients
- The Plan pays performance penalties for failing to accomplish installations correctly, completely and timely - and has no convenient means to reverse the trend
- Critical steps - such as post-sale underwriting and an end-of-process quality reviews - might not occur - leaving the Plan with problematic accounts and/or data to deal with downstream from the installation process
2. Embedded Process Problems
The end-to-end Client Installation process often suffers from a host of problems that need to be corrected by process improvements, increased automation and other methods. Some of the typical significant issues are:
- The Plan's Operating units have little or no visibility into the sales and renewal pipeline, or into the product development/management/change process - which prevents them from preparing themselves to receive and effectively manage changing volumes of work and work content due to membership increases and product changes about which they have not been informed. This lack of visibility often leads to:
- Errors in handling new products and new product changes due to the insufficient education and training of the operational staff
- Reactive capacity planning - resulting in excessive uses of overtime and temporary help
- Bottlenecks in the work flow - as workloads and arrival rates get out of sync with available staff
- Sales staff attempting to intervene on behalf of their "important" clients - this 'expediter' behavior is counter-productive to overall throughput
- Clients and their agents are habitually late in submitting group and member data - and do not Quality Control it - many clients utilize multiple benefits providers to serve the needs of employees, retirees and dependents. Clients often make benefits decisions on their own schedule without regard for what the benefits providers - including Health Plans - desire. Each benefits provider has a different way of doing business and a different timing cycle for when they want to receive data from the account. Clients and their third party agents - from brokers to benefits consultants, to payroll and HRIS processors to total benefits outsourcing vendors - do not always understand how the Plan's processes work and how they could positively or negatively impact its flow and results. When clients and their agents send or electronically transmit data late or incompletely or erroneously, the Plan's sales and operating units receive such inappropriate data and must either disrupt their own processes to handle it or reject it back to the client or sales staff, which delays the installation
- The Plan's Sales staff also might be habitually late in submitting group and member data - and do not Quality Control it - the operating units receive incomplete and erroneous data from their Sales teams and either disrupt their own processes to handle it or reject it back to the client or sales staff which delays the installation
- Sales staffs are usually reluctant to send erroneous data back to clients - placing an inordinate problem resolution responsibility on the Plan's operational units
- Incomplete and erroneous data are caught too far into internal Plan processes - literally forcing the Plan to handle rather than reject it
- Too little - and "dirty" - automated enrollment and maintenance transactions via EDI and the Web - despite the Medicare Electronic Claims initiative in the early 1990s, the Workgroup on EDI (WEDI) in 1993-4 and HIPAA legislation in 1996, the industry is still awash in paper. Plans receiving paper-based group and member data spend excessive time and money on non-value-adding processes for inventory control, management of workflow and attendant documents and interpretation of data. Plans receiving incomplete, poorly formatted and/or erroneous electronic data - who then choose to correct it rather than send it back to the creators of such data - also spend too much time and money on what should be a straightforward, automated process
- The end-to-end process is excessively manual in nature - aided and abetted by systems that were built on "human-in-the-loop" design principles that force staff to correct basic errors and make mundane decisions that could and should be automated. These "human touch" processes lead to data transposition errors, correction cycles, process delays, process variability, inconsistent results, non-compliance with agreements, and, with too many people involved in the processes, excessive costs
- The set-up and maintenance of essential production data is often error-prone - the major internal goal of the end-to-end Client Installation process is the creation and maintenance of timely, sufficient, accurate and trusted production databases or data stores that contain account, member and benefits data of various kinds. When Plans execute the collection of processes and sub-processes that make up Client Installation in an un-managed way, they often introduce errors and inconsistencies in Account and Membership databases, as well as in the systems that store the benefits/product rules that govern:
- Providers' verification of coverage and benefits at the point-of-care
- Patients' ability to receive timely care in the right settings
- Billing, collection and premium accounting
- Claims processing, and
- Customer service.
3. Ineffective Coordination with Other Products & Product Providers
Finally, the Plan's Sales/Renewal, Product Management and Client Installation processes must be synchronized with providers of other benefit products and services that enhance the Plan's offerings. With regard to Client Installation, the Plan must coordinate all aspects of the sales/renewal program with all such external or internal benefit providers to assure that the end-to-end Client Installation program is complete, accurate and timely - on or before the effective date - across all parties' systems and processes. Until the last benefit in the chain is able to be used by members, the process is incomplete and ineffective from the customer's perspective.
Basic Components of an Effective Client Installation Program
In our experience working with Clients who wish to significantly transform and improve their performance in Client Installation, we have determined that effective solutions require at least the following four (4) major components:
- Horizontal Process Alignment with a Single Point of Ownership and Control
- Significant Behavioral Changes
- Appropriate Visible Metrics, Reporting Mechanism(s) and Controls,
- Processes and Systems Engineered to Produce Right Outcomes
In the following sub-sections, we briefly outline what is required in an effective program. Questas would be happy to work with you and your team to diagnose your current operation and suggest and help implement a program tailored to your Plan environment.
1. Horizontal Process Alignment with a Single Point of Ownership and Control
The Plan's major business units that provide components of the Client Installation process need to agree to view and manage - or allow management of - the Client Installation flow as a single, discrete, horizontal process that cuts across their many individual organizational silos.
Additionally, the unit leaders need to agree to appoint or have appointed a controlling mechanism that has single point of ownership and control over the process. In our experience, that single point of ownership and control could be:
- An individual executive in the role of Process Owner - this is the solution that best fits in an organization that has committed to moving or has moved to a process-focused model. Client Installation is the epitome of the discrete end-to-end horizontal process. Once a process-focused Plan recognizes this concept, it is intuitive that Client Installation needs to be managed by a single process owner
- A Program Management Office (PMO) - comprised of a small team of knowledgeable, experienced professionals who can set up and operate a 'command and control' function to launch and implement a successful Client Installation program. Once the process has been institutionalized, the PMO will either shift its responsibilities to a single Process Owner as above, or become the operational entity that drives this process going forward
- A 'War Room', which is a specialized form of a PMO - in some Plans, "PMO" has become an undesirable term, e.g., due to PMOs' visible involvement in past projects that were problematic or failed. In such cases in the past, some of our clients have utilized the metaphor of a War Room - or Situation Room - as the command and control function. Since the terms "War Room" and "Situation Room" conjure up visions of staffs working through crisis situations together, some Plans find this terminology to be quite appropriate for a newly recognized horizontal process - like Client Installation - with such important market-visible outcomes. War Rooms operate like PMOs
The various business unit leaders need to cede to their single point of ownership and control both the authority and responsibility to implement and manage the horizontal Client Installation process on their collective behalf. This usually requires significant behavioral change at the senior management and executive levels - and is often the hardest issue to overcome in order to implement an effective program. Questas' organizational behavior and design consultants often intervene in these situations to coach leaders through the transitional stages necessary to this process.
Finally, business unit leaders need to agree that they will realign all or portions of their performance management, compensation and reward systems to motivate their staffs to behave properly, effectively and timely in meeting the cross-silo objectives of the horizontal Client Installation process. Their staff needs to understand that this is a critical Plan function that must be done well and on time.
2. Significant Behavioral Changes
In addition to the behavioral changes required of the Plan's leaders, the staff members in each silo who participate in the Client Installation program also need to alter their behaviors and their process-oriented reporting lines.
The Client Installation 'owner' controls and dictates the priorities for the end-to-end Client Installation program. Staff in each silo becomes accountable to the Client Installation owner for managing work flow and controlling inventory, meeting deadlines, making appropriate decisions, achieving target quality levels and delivering the right results. As with the leaders, the staff needs to re-orient their behaviors and, for the purpose of this process only, their reporting lines to help assure the success of the horizontal cross-silo process.
Interestingly, in some instances in our experience, this represented the first time that the sales, underwriting and operations staffs had ever closely collaborated on a core process, on a daily basis and with the same collective objective. Cross-silo collaborative behavior must be learned - and often takes some time to be assimilated by the various staff members. Some may need coaching - others will not.
The Plan's leaders need to continuously reinforce the importance of working and behaving in new ways to create successful outcomes on behalf of the Plan's group clients and members - and not provide a convenient 'out' for staff who do not wish to cooperate.
3. Appropriate and Visible Metrics, Reporting Mechanism(s) and Controls
As with other processes, the Client Installation process must be accompanied by an appropriate set of target service levels and metrics - both external and internal. They should be transparent to the staff, reported often, and the team should be motivated to continuously improve performance against them. Some of the key metrics are as follows:
External Target Metrics - those that are visible to and valued by clients - examples:
- 100% of all new and renewing clients and members installed correctly and
completely on or before the effective date of the client (or individual)
- In some Plans, "effective date" might be changed to a promised date beyond the effective date for certain types of business - e.g., late-deciding small businesses
- For Plans that have not used or assessed and reported this end-to-end metric before, the first month's as-is results are sometimes startling - as low as 54% in our experience. But the path of progress should then be steep - yielding results that quickly reach the mid-90% range and improving
- Minimal to no financial penalties paid for failing to meet the key metric above
- Renewal packages delivered to the account, third party intermediary or non-group client on or before target date, which itself depends upon the type of business and its requirements
- All collateral material - ID cards, handbooks, certificates, contracts, etc. - accurately reflect what the client 'bought'
- Timely, accurate initial and follow-on bills - with targets for each
- Timely, accurate initial and follow-on commission payments - with targets for each
- Accounts and their agents and members are 'happy' with the process - which the Plan measures on a regular basis
Internal Target Metrics - those that are visible to and valued by the Plan itself - examples:
- Account, member and benefit databases/data structures are timely, accurate, sufficient and trusted data sources - yielding fewer root cause problems for other Plan processes
- Account terminations and member 'back-door' losses for the expressed reason that the initial installation was problematic or a failure (provided via an objective exit interview) continue to decline to or below given targets
- Complete and accurate renewal packages delivered on or before target dates
- Rate changes and benefits are confirmed and implemented for all groups
- No financial penalties paid for failing to meet the 100% installation target
- Clean, quality controlled data received by operations from clients and/or sales entities exceeds a threshold %-of-clients level (and improves over time)
- Each silo unit meets its throughput, cost and quality goals while the overall process meets the 100% installation target
- All units perform at or below target overtime and temporary help budgets
- Costs per enrollment for both groups and members meet or beat targets
- Urgent client installation problems get resolved expeditiously without bureaucratic delay
- No groups or members "fall through the cracks"
- Eliminate cost of re-work due to late installs and retroactive actions (premium re-billing, claims reprocessing, etc.)
- Web/EDI/other automated enrollment achieves target levels for volumes, quality and timeliness
- Reduced lapse rates (at or below target %) for both accounts and members - measured over a long period of time
- Lapsed groups do not receive benefits past the termination effective date
- Increased 'show' rates among brokers, benefits consultants and other sales channels. The 'show rate' reflects how often the sales entity introduces or 'shows' the Plan's products and prices to prospective buyers - the higher the rate the better
- Lower cost of sales
- Increased profitability/surplus - driven by '[initially and] continuously happy clients'
In addition to the key metrics, the Client Installation program often requires new process controls to address and gain control over such undesirable events as randomly arriving group and member data, account needs that should have been defined at the time of the sale or renewal, surprise product and service changes, group and member data arriving without having been quality controlled for completeness or correctness; etc. These items are unique to each Plan and should be defined and implemented as needed by the Plan.
4. Processes and Systems Engineered to Produce Right Outcomes
As noted in the next section below, once a Client Installation program is approved and the as-is diagnosis of the current policies, practices and methods is underway, the Client Installation team will almost without fail determine that:
- Some of the Plan's related processes need to be immediately improved or re-engineered over time, and/or
- The Plan's systems need certain changes, and/or
- Some processes would benefit from increased automation and less manual work.
While the end-to-end Client Installation process could be made to work without such interventions, they would make the process more effective, less costly and less manual over time and should be addressed when and as resources can be freed up to do so.
It is also important to note that Client Installation programs are sometimes implemented while a Plan has ongoing business process improvement/re-engineering and/or system implementation initiatives in progress. Plans sometimes wonder if a Client Installation program and these process improvement and systems efforts are redundant and duplicative - most often they are not.
When insurers and HMOs undertake the re-engineering of some or all of the processes in the silos that, collectively, could or should make up the horizontal flow of the Client Installation program, the processes are usually addressed within each silo - sometimes between a few silos. The as-is effort uncovers root cause problems within the silo and those caused by preceding silos. And meaningful improvement often occurs to the silo tasks.
However, because most Plans and consulting entities do not view or treat the horizontal Client Installation process as a single core process with major market-driven and internally-driven outcomes, the end-to-end process is almost never considered or addressed in its entirety - unless, of course, Questas is doing the process improvement work for the Plan.
Thus, when the Client Installation program is launched, the Client Installation team can provide new insights and improvement opportunities for the individual process teams to assess and address. The team can cause the process teams to view their own work in a broader context - which positively influences how they define issues and opportunities, look for root causes and determine the effects of process outcomes on other Plan functions - like billing, claims and customer service, which otherwise might not be addressed in silo-oriented re-engineering efforts in sales, underwriting and/or account installation.
Similarly, the Client Installation team will propose new ideas to be considered for enhanced process automation - from controlling and reporting on sales and renewal pipelines from identification through implementation, to improving EDI and Web-based processes, to automating the entire Client Installation process from end-to-end. The Plan will then have to determine its appetite and budget for such new concepts and implement accordingly.
Implementing an Effective Client Installation Program
Since most Health Plans have not [yet] adopted a process-focused business model, we would recommend that they implement a new Client Installation program around the Program Management Office (PMO) or War Room model.
For those Plans who are adopting or have adopted a process-focused structure, we recommend making Client Installation a core process that reports to a single Process Owner who will then drive a program similar to what we describe below.
For convenience sake in the remainder of this section, we will use a PMO/War Room structure and call it the Client Installation Command Center or "CICC." The changes to be made to accommodate a process-focused environment should be intuitively obvious.
If a Plan undertakes this program alone, or engages a knowledgeable and experienced firm like Questas to assist it, the program would typically unfold as shown below. The list of tasks would occur while each physical Client Installation Command Center or Centers was being assembled and staffed:
1. Gain an understanding of the current organizational structure
2. Establish or re-affirm buy-in at highest level in the Plan
3. Gather data and conduct a rapid as-is of the current flow as the basis for establishing the physical CICC - validate findings in workshop(s)
- Gather anecdotal information as well as key metrics data
- Analyze current performance - determine how the Plan performs against a set of defined or experience-based 'ideal' metrics - note gaps
4. In rapid fashion, define the immediate "to-be" client installation process for the organization, focusing on key outcomes for accounts, members and the Plan
- Make basic alterations to the as-is configuration as necessary to accommodate the new Client Installation program
- This is not a business process engineering design - it addresses immediate changes that will benefit the process - example: running small businesses and large businesses through the operational areas in parallel so neither is disadvantaged by work for the other
5. Review the initial 'to-be' client installation process - accompanied by the necessary authority, responsibility and control mechanisms and provisions - with Plan executives, process owners, key IT staff and other key players - and gain final approval to implement
- Introduce the CICC concept and each person's role in the new process
- Create/distribute easy to use process aids for all affected departments
- Communicate requirements for - processes, data, timing, results, reporting responsibilities and times, etc. - to all affected departments and staff
6. Create new or modify existing tools (electronic if possible) to include
- Process maps showing the new to-be flows, each process, its timing, characteristics, key owners and players
- Progress tracking mechanisms - overall and at sub-process levels
- E-documents and other methods for inventory management and controls within and between departments
- Daily/weekly/monthly status media, scorecards and performance dashboards
7. Kick-off the CICC - commence gathering of tracking data from all business units and begin the command and control program
8. Once underway, identify and implement approved business process improvements/re-engineering opportunities and systems changes
After the CICC has been implemented, its roles and responsibilities are shown, in overview fashion, in the graphic below:
As noted earlier, the CICC - in the form of a PMO or a War Room - is comprised of a small team of knowledgeable, experienced professionals who have set up and operated this 'command and control' function to implement the now-successful Client Installation program. Once the process has been institutionalized, the CICC will, at the Plan's discretion, either transition its responsibilities to a single Process Owner or actually become the ongoing operational entity that drives this process in the future.
In the collective experience of several of the Questas consultants who have helped medium- and large-sized Health Plans implement this type of program on 7 occasions, well-conceived Client Installation programs are usually able to be set-up and operable within a short 2-3 months of the start date and generate real, measurable benefits immediately thereafter.
Further, our experience suggests that each PMO/War Room is:
- In actuality a shared service center for the Plan, requiring a governance structure and a charter that might be foreign to the Plan's usual way of doing business
- Usually staffed by 2-4 qualified individuals one of whom is senior in nature - Director or Vice President if a Plan resource, and a Principal or Senior Manager if from the consultancy
- Most often launched and initially managed by a consulting team which mentors Plan staff until they are ready to assume control following a well-defined transition program
- A rapid method for getting to meaningful, market-visible results before any significant monies are invested in core process engineering and new systems automation
- An excellent, new and innovative way for a Plan to demonstrate its commitment to service excellence to new and prospective clients
Summary of Timing & Benefits
As noted in the previous section, a well- conceived Client Installation program should allow the CICC to be set-up and operating within a short 2-3 months of the start date and should generate real, measurable benefits immediately thereafter.
A properly implemented Client Installation program should create significant benefits for a Health Plan and its clients - both accounts and members. Some of these benefits are near-term and measurable and should be part of the Plan's assessment of Return on Investment (ROI) for the process. Others are either more qualitative or 'softer' or require long periods of time to become evident (such as the effects on lapse rates).
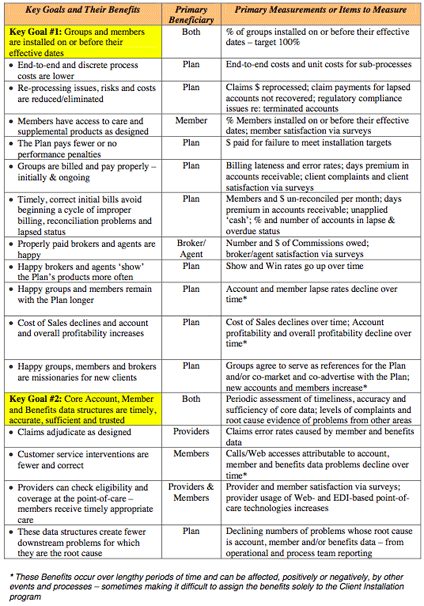
The benefits inure to the parties based on the Plan's ability to achieve two Key Goals represented as the major external and internal performance targets:
- Install 100% of all accounts and members correctly and completely on or before their effective dates
- And create and maintain timely, accurate, sufficient and trusted core production data structures for account (includes billing), member and benefits data
We have tabularized the Key Goals, key benefits and their measurement criteria for the reader's consideration.
Conclusion
Once the sale is completed, Client Installation represents the first time a new client experiences a Plan's services platform. For renewing clients, it can either be a reminder of the services it has experienced before or signal a new - positive or negative - trend in Plan services. The impression left by the client installation event is lasting and certainly affects decisions by accounts and members to remain with the Plan over time or to 'lapse.'
"Profit equals revenue from continuously happy clients, minus costs." (Tom Peters, "Thriving on Chaos")
Peters' mantra might be at the core of your Plan's service philosophy or represents a new concept you wish to consider for the future. Either way, it is clear that an unhappy and frequently churning account and member base costs more to service, saps scarce resources, erodes profitability and reduces the numbers of reference clients for new sales efforts.
It is also clear that failure to properly capture account, member and benefit data during the installation process and to store them in timely, accurate, sufficient and trusted data structures impedes the Plan's ability to prosecute its operational business effectively and efficiently - thereby eroding the client's confidence and the Plan's profitability.
Many Plans do not manage Client Installation as a critical discrete horizontal process - and often suffer the effects noted herein. The process is too important to be left to chance, to the good will of the Plan's staff, or to hordes of temporary help depleting your overtime budgets.
Questas can assist you and your staff in better understanding and improving your approaches to Client Installation. We can be reached at client-installation@questas.net or by calling us at 212.229.0498.
Print or Download
Download this document in PDF format to print or read off-line.